Desperate for relief, many people living with inflammatory bowel disease (IBD)—either Crohn’s disease or ulcerative colitis—rely on biologic therapies that require users to self-inject. Because self-injecting can be a daunting task—evidenced by the 45% of patients who skip or altogether avoid injections due to anxiety or fear—proper training and onboarding is critical. Even more alarming is that nearly 50% of healthcare providers (HCPs) neither receive training themselves, nor train their own patients, on how to properly administer a self-injection.
In one study specifically focused on IBD patients, just over two-thirds of respondents (67%) said that if given a choice between receiving two monthly intravenous infusions at an HCP’s office or self-injection every other week at home, they would prefer the former because they “do not like the idea of self-injecting.”
Given this response, and as the use of self-injectable therapies continues to rise, it is increasingly vital that HCPs understand patients’ comfortability with self-injecting. A high-quality standard of training and onboarding must be established to avoid injection errors, reduce anxiety and take the guesswork out of self-injections. What’s more, 86% of patients make errors with autoinjectors—a sobering statistic that must be addressed. Injection errors are especially hazardous because an underdelivered dose may be ineffective, and according to the Crohn’s and Colitis Foundation of America (CCFA), an estimated 75% of people with Crohn’s disease will require surgery, especially if their medication is ineffective or if their condition has worsened.
Currently, most IBD patients complete one initial in-office training session with their new injectable and are then on their own for the course of the treatment. How well they self-inject in the privacy of their homes varies significantly. Research suggests adherence success may depend on whether the prescribed treatment is supported by training materials that go beyond an introductory in-office session and the standard Instructions for Use (IFU).
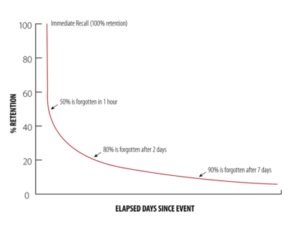
Studies also find that patients’ own natural memory decay, coupled with longer periods of time between injections, further highlights the need for training devices in the home to use throughout treatment and not just one time in an HCP office.
In fact, a recent longitudinal study—in which researchers sought to understand how patients interact with training devices—uncovered encouraging statistics for the case for trainers. A whopping 100% of study participants who were given training devices to practice with at home successfully completed all crucial self-injecting steps after a two-week practice period. In contrast, more than half of participants without training devices made critical errors.
Patients want these additional resources and support to feel more confident at home. One study finds 92% of patients prefer to receive and practice with training devices at home. With even more support, such as formal patient support programs, adherence rates to therapies skyrockets to 94%.
Training devices have made such an impact with patients because they incorporate a range of high-tech features to create realistic practice self-injections. High-quality trainers replicate the drug viscosity, plunger speed and feel of the injector tip on the skin, as well as the audible feedback that mimics the sound of an actual drug delivery device. With these training devices, an overwhelming 86% of patients report increased confidence in self-injecting, thus increasing adherence and overall outcomes.